As Prisma doctor's new invention could save lives, DHEC projects 8,000 S.C. cases by May
Hospitals registering 3D printer can use device that splits a ventilator for use by four patients
kayla@theitem.com
Wednesday saw a flurry of funding, innovation and demographic data in response to the coronavirus' continued expected spread, including an invention from a Prisma Health ER physician that allows a single ventilator to support up to four patients.
Prisma Health's new VESper received emergency use authorization from the U.S. Food and Drug Administration, health care system officials said Wednesday, and they are making the code available for free to anyone who registers their 3D printer. Deployed with 3D printer technology, the device is developed with material already in use for medical devices.
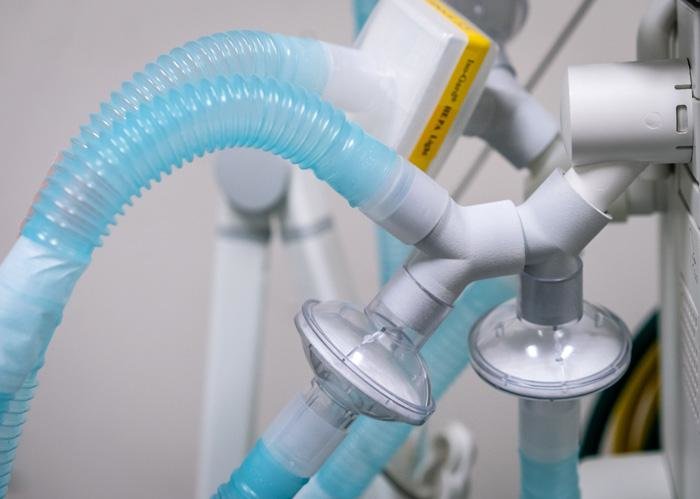
The VESper, which stands for ventilator expansion splitter, does that just. The device attaches to the ventilator circuit and splits the flow to four different patients as opposed to one, according to Peter Tilkemeier, chairman of the Department of Medicine at Prisma Health-Upstate.
Sarah Farris, an emergency room physician in the Greenville hospital and a clinical faculty member at the University of South Carolina School of Medicine in Greenville, came up with the idea and asked her software engineer husband to write code for it with help from a Prisma Health pulmonary critical care physician.
"When we see rapid increases in patients who require machine-assisted breathing, an acute shortage of necessary equipment can happen overnight," Tilkemeier said.
The "y" splitter tubing device is being promoted as lifesaving when the number of critically ill patients requiring breathing support to survive is greater than the number of available ventilators. Tilkemeier said a number of hospitals in the United States are likely to begin experiencing this with COVID-19.
Marjorie Jenkins, chief academic officer for Prisma Health in the Upstate market and dean of the USC School of Medicine in Greenville, said engineers at Clemson University and USC printed prototypes, and the Prisma team began working to secure FDA approval, which came together in a matter of days between the end of last week and beginning of this week.
Hospitals can apply to receive the free source code and printing specifications for the device now by registering at www.prismahealth.org/vesper.
Prisma is working with major companies such as HP Inc. to quickly scale 3D production of validated parts for distribution in areas of greatest need and areas with the potential to exceed their ventilator capacity in the near future. Those COVID-19 “hot spots” are designated by FEMA.
Critical need, Tilkemeier said, means a facility is out of available ventilators and a patient will otherwise die from the virus’ respiratory complications.
Tilkemeier said hospitals throughout South Carolina currently have enough ventilators available for patients.
STATE AT 7 DEATHS, 424 CASES
As health care facilities continue preparing for increasing numbers of positive cases, a question that remains across all communities globally is what is the breaking point? When will health care systems become overwhelmed with patients as seen in China, Italy and, increasingly, New York?
The S.C. Department of Health and Environmental Control released projections Wednesday that the Palmetto State may see a total of more than 8,000 cases by May 2, taking into account that extreme social distancing, its opposite, delays in lab reporting, increased numbers due to increased testing and the virus’ reported distaste for warm weather may sway the projections one way or the other.
DHEC announced 82 new cases on Wednesday, including two more in Sumter, bringing the total statewide to 424 across 39 counties. Shaw Air Force Base announced a second case in a Team Shaw member.
There have also now been seven deaths, including one in Sumter, two in Florence and one each in Clarendon, Lexington, Charleston and Horry.
Providing new provisional data Wednesday, DHEC reported the age group with the highest percentage of patients so far in the state has been those aged 61-70, with 19% of the total cases being in that range. Following cases by age group are 51-60, 41-50, 71-80, 21-20 and 31-40.
The average and median age of the positive cases so far are both in the low- to mid-50s, with patients ranging in age from 2 months to 93 years.
The gender breakdown is about split, with 49% being male, 48% being female and the remainder unknown, according to DHEC. So far, 54% of the patients have been white and 39% African-American.
At the time of illness, 24% required hospitalization.
FINDING MORE SPACE TO PREPARE FOR FUTURE NEEDS
An interactive map using data from Kaiser Health News distributed by the Associated Press to its member media outlets breaks down the number of ICU beds in every county in the nation. Data show more than half the counties in the U.S. have no hospital ICU beds, mostly seen in the middle of the country and mid-northwest.
The map shows Sumter County with 17 ICU beds, Clarendon County with six, Richland with 211, Kershaw with 10 and Lee with zero.
Those 17 beds in Sumter are at Prisma Health Tuomey Hospital. Hospital officials confirmed the number and said they are working to free up four more ICU rooms that were being put to different uses.
An NPR analysis of data from the Dartmouth Institute for Health Policy and Clinical Practice examined how ICU beds are distributed across 304 markets (not necessarily counties) carrying the nation’s 100,000 ICU beds. According to the analysis, Florence has 62 ICU beds per 100,000 people, the fourth most in the nation. The Kaiser map shows Florence County has 98 total ICU beds.
When searching Sumter, the Dartmouth data show Columbia has 42 ICU beds per 100,000 people, ranking 55th out of 304 hospital referral regions.
“As all hospitals are doing, we are looking at plans to open units that may have been temporarily closed because patient volume was down. That’s a normal occurrence, as patient volume routinely fluctuates,” said Robbie Gainey, manager of the ICU at Tuomey.
Gainey said Tuomey has an 18-bed unit they are ready to open if needed.
Not every person who has the virus needs hospitalization, a ventilator and/or an ICU bed.
“Others may need a hospital bed because they have viral pneumonia and require supportive care. Some people may not be able to breathe well on their own and may need to be on a ventilator; that is something that could elevate you to the ICU floor,” Gainey said.
The difference between a regular bed and an ICU bed is that ICU beds have monitoring capabilities bedside in addition to the nurse’s station, Gainey said. Tuomey ICU beds also have a “broader range of monitoring practices.” The biggest difference, he said, is the additional training of the nursing staff and physicians.
Other health care centers throughout South Carolina are also working to free up space for critical needs.
MUSC Health plans to use recently vacated critical care space in the old Children’s Hospital, now known as University Hospital Extension, as well as possible ICU space in Ashley River Tower for about 100 extra beds.
According to Heather Woolwine, director of MUSC Public Affairs, Media Relations and Presidential Communications, the system is working with regional health network hospitals in Florence, Marion, Chester and Lancaster to plan for surge capacity.
To prevent more cases from spreading, Clay Lowder of Colonial Healthcare urged people to stay home, saying this is a critical week in ensuring medical facilities do not get overwhelmed.
The term “flattening the curve” has been used to describe how quickly cases escalate and gives two scenarios. One is that we see a dramatic, sharp increase, burdening hospitals and health care facilities. The other is a slower, more steady count of new cases, keeping the case load within the range of what health care facilities can handle over a longer period of time.
Lowder said on Tuesday that Colonial has tested positive 10 cases. DHEC’s reporting is by its nature behind local facilities because tests must be sent to DHEC and confirmed before being reported.
More Articles to Read